How to Make a Referral?
Please call our our TMS coordinator, Camice, at 719-359-8812. Alternatively, you may wish to ask your patient to fill in the contact form at the bottom of the page, to gain access to our medical history questionnaire.This questionnaire gives us the basic information insurance companies require for submittal.Without such detailed information, most insurance companies will not agree to pay for TMS.
Is a referral letter needed? What else?
If the patient can get a printout from their pharmacy, this may speed up your process. They should request that it extends back the maximum number of years possible.
We will need a referral letter from you. Please include:
- The patient’s diagnosis
- The reason for the referral (such as mediation failure or intolerance to medication side effects)
- Patient history with a much detail as you can including
- Each medication given to the patient
- The exact doses given
- Start and stop dates
- The impact of the medicine
- The patient’s side effects, if any
How Does TMS Therapy Work?
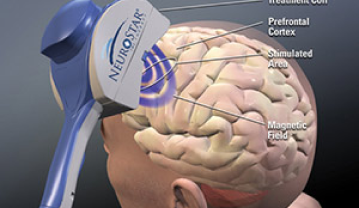
Through non-invasive treatments, TMS stimulates nerve cells in the area of the brain that regulates mood
TMS delivers MRI strength (1.5 Tesla) magnetic energy to the region of the brain that is targeted. The magnetic energy acts directly only at a small area of the cortical surface.The target is selected based on the condition being treated. In the case of MDD, this will be the left Dorsolateral Prefrontal Cortex (DLPFC).
In depression, the left DLPFC is under-active as seen on both EEG and fMRI studies. Deeper structures are also underactive.The fluctuating magnetic field induces action potentials along the axons of the underlying neurons. This leads not only to immediate release of neurotransmitters but also to adjustments in neurotransmitter receptor site densities.Since the DLPFC has many neuronal connections to the ipsilateral and contralateral limbic and hippocampal structures, simultaneous alterations in brain activity occur in these deeper structures with each treatment. TMS leads to alterations in these functions over time as long term potentiation occurs.
What Types of TMS Do You Offer?
At Southern Colorado TMS we stay current with the rapidly changing TMS field. We have experience with three of the FDA cleared devices and currently use the best tolerated and most comprehensive third generation machine.
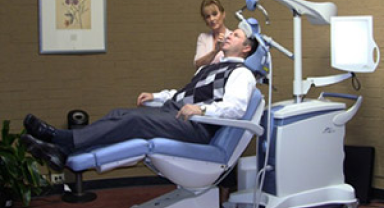
Based on this extensive experience and ongoing discussion with TMS providers across the US we will select the technology which offers best fit between efficacy and comfort for your patients. Our Medical Director will then select the most relevant treatment protocols for each.
Each TMS treatment has flexibility in targeting the coil to the brain regions that need stimulation. The electromagnetic field in rTMS extends about ½ way through the cerebral cortex. The DLPFC is a primary target and is highly interconnected with deeper brain structures involved with depression.
But research has expanded dramatically since 2008 with remarkable results, some currently under FDA-review with potential treatments for PTSD, autism spectrum disorders, stroke rehabilitation, Alzheimer’s, the depressive aspect of bipolar disorder, OCD, migraines, tinnitus, ADD, and treatment of teenagers suffering from MDD.
What are the Patient Costs for TMS?
How long does it take TMS therapy to begin to work?
Almost all insurance companies cover TMS treatment for MDD but not yet for other diagnoses. The primary exception is Colorado Medicaid. We do accept Medicare. Tricare coverage is available, as well as most other commercial insurances.
Most insurance companies require a prior authorization which we will obtain. Each requires a different history of failures of previous medications in order to pay for TMS treatment. A general rule of thumb is that four medications of different classes and either adequate dose and duration or intolerable side effects are required. Sometimes an augmentation trial must be demonstrated but we have been successful in obtaining authorizations where some of these were lacking.
Will the patient need to pay a copay?
Most insurance plans do require a copay to be paid. If the patient has not yet met their plan deductible for the year this may also be owed. We will work with your patient to obtain an estimate. We typically require patients to make copayments in pace with services. Plans may pay TMS from either medical or mental health benefits sides of their ledger, making advance estimates of how TMS will be paid difficult at times. HSA (health savings accounts) pay for TMS. Financing referrals are available but with increased coverage this is seldom necessary. We will work hard to make treatment possible for your patient
Why Should I Refer to SCTMSC?
We are here to make a difference and will always do what we can to assist you and your practice. Let us know how we can help you and, above all, your patients.
Best experience and training
- Providing TMS services since 2011
- Over 300 patients evaluated and treated
- Medical Director has been involved with and studied TMS since 1995
- All technical staff trained and/or certified to the standards of Neuronetics, Brainsway and MagVita
- A clinic staff of 8 (and growing) to assist you
Best patient care system
- TMS support and education groups for all patients at no charge
- Affect management training using Heart Math at no charge
- We are here to make a difference and will always do what we can to assist you and your practice
- Let us know how we can help you, and above all, your patients
Best technology
- Offering both the MagVita and Neurostar systems of treatment
- EMG and EEG services available on site
- Patient status monitored during treatment and for 12 months afterward
Best interface
- Effective relationships with all prior authorization systems
- In network or single case agreement relationships with most major insurance carriers


